Meth sores are painful, often disfiguring skin lesions that develop in people who use methamphetamine regularly. They are not caused by a single factor but by a combination of how meth affects the brain and nervous system, how it damages blood vessels and immune function, and the skin picking and infections that follow. Understanding what causes meth sores, how serious they can become, and what recovery looks like can help individuals and families recognize the problem early and seek treatment before permanent scarring occurs.
Key Points
- Multiple causes, not one: Meth sores result from formication (the sensation of bugs crawling on skin), compulsive picking, poor wound healing, weakened immunity, and bacterial infections – not from meth being “dirty” or a single toxin.
- Serious infection risk: Research shows meth users have significantly higher rates of methicillin-resistant Staphylococcus aureus (MRSA) and other dangerous skin infections that can spread and require hospitalization.
- Healing requires stopping use: Medical care can treat individual sores and infections, but sores will keep appearing as long as meth use continues because the underlying causes – the picking, poor healing, and immune suppression – persist.
- Recovery is possible: Once someone stops using meth and enters treatment, skin gradually improves over weeks and months as the body’s natural healing processes resume and immune function recovers.
What Are Meth Sores and Where Do They Appear
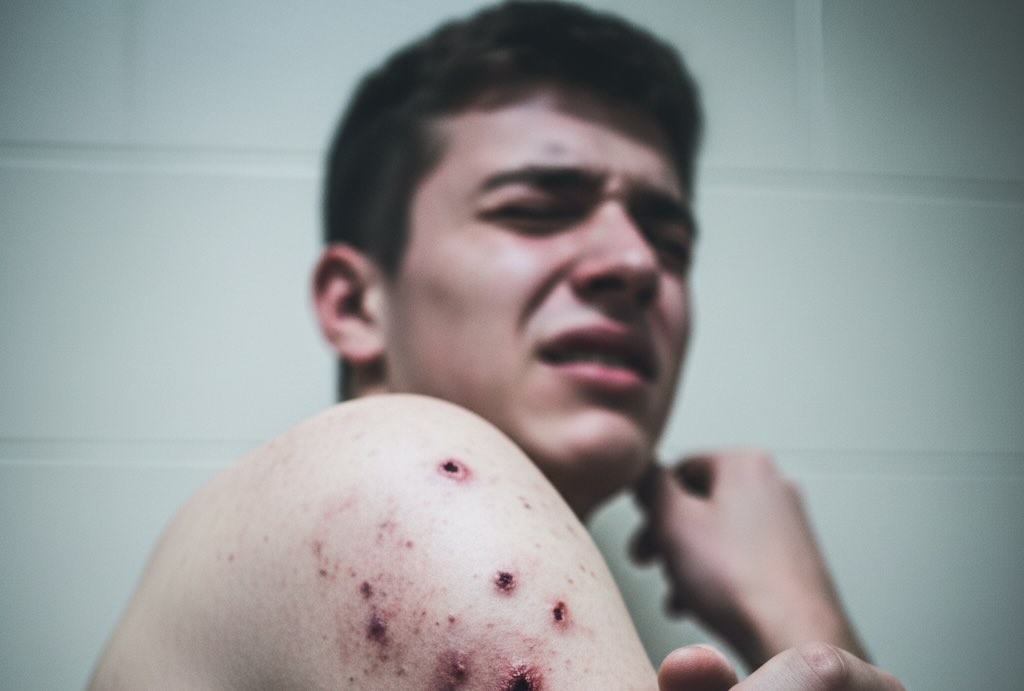
Meth sores are open wounds, crusted scabs, and scarred patches that develop on the skin of people using methamphetamine regularly. They are not a rash or a single type of lesion but a collection of wounds at different stages of healing – some fresh, some crusted, some already scarred. The sores tend to cluster on areas a person can easily reach and pick at repeatedly: the face, scalp, neck, arms, hands, chest, and upper legs.
Many people describe the sores as concentrated around the cheeks, jawline, forehead, and nose, which leads some clinicians to call the overall appearance “meth face.” But the sores do not stop at the face. Anyone with heavy meth use can develop them anywhere on the body where scratching and picking occur. Some people have deep, crater-like scars from large infections, while others show a pattern of smaller puncture-like marks from repeated digging at the skin. The variation depends on how long someone has been using, how hard they pick, whether infections have occurred, and how their individual skin responds to injury.
How Meth Causes Skin Damage – The Three-Part Process
Meth sores do not appear by accident. They result from a three-part process driven by how methamphetamine affects the brain, blood vessels, and immune system.
Part 1: Formication and Compulsive Skin Picking
Methamphetamine is a powerful stimulant that floods the brain with dopamine and norepinephrine. At high doses or with chronic use, meth can trigger hallucinations and abnormal sensations. One of the most common is formication – the sensation that bugs or insects are crawling on or under the skin, even though nothing is actually there. This sensation feels extremely real to the person experiencing it and drives them to scratch, dig, pick, or squeeze their skin to try to “get the bugs out.”
This picking starts the damage cycle. A person might scratch a completely normal area of skin, creating a small wound. But the urge to pick does not stop. The formication continues, the person scratches again and again at the same spot, and what began as a minor abrasion becomes an open sore.
Part 2: Poor Wound Healing and Weakened Immunity
At the same time meth is driving the picking, it is also damaging the body’s ability to heal wounds normally. Methamphetamine narrows blood vessels throughout the body, which reduces blood flow to the skin. Less blood flow means fewer nutrients and oxygen reaching injured areas, so healing slows dramatically. What might normally take a few days to scab over can take weeks or longer in someone using meth regularly.
Meth also suppresses immune function. Research has shown that meth exposure interferes with white blood cells and other parts of the immune system that normally fight bacteria and prevent infection. This double hit – slow healing plus weak immunity – creates a perfect environment for bacteria to invade and multiply in open wounds.
Part 3: Bacterial Infection and Deep Sores
Once the skin is broken and immune function is compromised, bacteria colonize the wound easily. For many people, this is where meth sores become truly dangerous. Research published in medical journals has documented a strong link between methamphetamine use and serious skin infections, particularly those caused by methicillin-resistant Staphylococcus aureus (MRSA). Studies have found that among people presenting with community-acquired skin infections, meth use was present in a significantly higher proportion of those with MRSA compared to those without.
When MRSA or other dangerous bacteria take hold in an open meth sore, the wound can expand rapidly, become hot and very painful, and develop into a deep abscess that requires drainage, strong antibiotics, or even hospitalization. Some infections spread to the bloodstream, causing sepsis – a life-threatening condition. This is not a minor cosmetic problem. Untreated meth sore infections can become medical emergencies.
What Meth Sores Look Like at Different Stages
Meth sores progress through several stages, and someone actively using meth will often have sores at multiple stages on their body at the same time. Understanding what each stage looks like can help recognize the problem in a loved one.
| Stage | Appearance | What Is Happening |
|---|---|---|
| Early picking | Small red bumps or scratch marks that look like acne, bug bites, or minor scrapes | The initial wound from scratching. Skin is broken but not yet deeply infected. Person may say they were bitten by bugs or have a rash. |
| Active sore | Open wounds with redness and swelling around the edges, sometimes oozing clear fluid or pus | The wound is continuing to be picked at. Healing is slow due to poor circulation. Bacteria may be colonizing the site. |
| Infected sore | Deep, crater-like lesion with thick yellow or greenish drainage, surrounding skin very red and swollen, area is hot to touch | Serious bacterial infection, possibly MRSA. This stage requires urgent medical attention. Infection can spread quickly. |
| Healing sore | Thick brown or black scab, sometimes with yellow edges. May be very large, covering an area of multiple centimeters | The wound is finally healing, but if meth use continues, it will just be picked at again. This stage can last weeks. |
| Scar | Pitted, depressed scar, sometimes shiny or discolored (darker or lighter than surrounding skin) | The wound has healed, but scarring is permanent. Continued meth use means new sores form nearby while old scars remain. |
The Serious Complication – MRSA and Other Dangerous Infections
Infection is where meth sores stop being just disfiguring and become life-threatening. Medical research has documented that people who use meth have much higher rates of skin and soft tissue infections compared to the general population, and a significant portion of those infections are caused by antibiotic-resistant bacteria like MRSA.
In one study examining community-acquired skin infections, researchers found that among patients with MRSA infections, methamphetamine use was significantly more common than among patients without MRSA. This is not coincidental. It reflects the fact that meth users have both open wounds (from picking) and compromised immunity (from the drug), making them vulnerable to serious infections.
MRSA is particularly dangerous because it is resistant to many common antibiotics. If someone develops an MRSA infection in a meth sore, standard antibiotics will not work. Treatment often requires more aggressive approaches such as draining the abscess, using stronger antibiotics like vancomycin, or in some cases hospitalization for intravenous therapy. If the infection spreads to the bloodstream, it can cause sepsis and organ failure.
Beyond MRSA, meth users with open sores are at risk for other serious infections including cellulitis (spreading skin infection), osteomyelitis (bone infection), and bloodstream infections. The poor hygiene often associated with active addiction – not bathing regularly, reusing contaminated items, living in unsanitary conditions – compounds these risks.
Why Meth Sores Do Not Heal Like Normal Wounds
A normal cut on the skin goes through a predictable healing process. Within hours, platelets form a clot and bleeding stops. Over days, immune cells clean up the area and new tissue begins to form. Within about two weeks, most minor cuts are scabbed over and healing well. Within a month, they are mostly healed and scarring is minimal.
Meth sores do not follow this timeline. Because meth narrows blood vessels and weakens immune function, the healing process is delayed at every step. The wound does not clot as efficiently. White blood cells are slower to arrive and less effective at fighting bacteria. New tissue does not form at a normal pace. A meth sore that should heal in two weeks might take two months or longer.
Meanwhile, the person is still using meth, still experiencing formication, and still picking at the wound – often before it has even started to properly heal. This means the damage keeps accumulating. A single area of skin might be picked at dozens of times, preventing any stage of true healing, and getting re-infected repeatedly.
Over months and years of active meth use, this repeated cycle of wounding, poor healing, infection, and re-wounding creates the characteristic pitted, cratered scars seen in people with long histories of meth use. These scars are often permanent, remaining on the face and body even years after someone stops using.
Treating Meth Sores – Medical and Behavioral Approaches
There is no special “meth sore cure,” but proper medical care can manage active sores and prevent serious complications while someone is working toward recovery.
Medical Management of Active Sores
For non-infected sores, the approach is straightforward wound care: gentle cleaning with soap and water, avoiding further picking, keeping the area dry, and using appropriate dressings (such as antibiotic ointment and bandages) to protect the wound as it heals. Topical antibiotics can prevent infection in minor wounds.
For infected sores, medical evaluation is urgent. A healthcare provider can assess whether oral antibiotics are sufficient or if the infection requires stronger measures such as drainage of an abscess or intravenous antibiotics. Wound cultures can identify which bacteria are present and which antibiotics will actually work. Without proper treatment, infections can worsen rapidly.
Some people also benefit from medications that reduce the sensation of itching or crawling feelings. While these do not replace treating the underlying meth addiction, they can reduce the urge to pick and allow wounds to heal somewhat faster.
Behavioral Support and Addiction Treatment
Here is the reality: no amount of wound care will prevent new sores from forming as long as someone is still using meth. The sores will keep appearing because the formication, picking, poor healing, and immune suppression will continue.
True healing of meth sores requires stopping meth use. And stopping meth use usually requires comprehensive addiction treatment – not just willpower. Treatment should include behavioral therapies (such as cognitive behavioral therapy or motivational interviewing), support for any co-occurring mental health conditions (such as depression or anxiety), and practical help with housing, employment, and social support.
Treatment can be inpatient, intensive outpatient, or standard outpatient depending on the severity of addiction and the person’s circumstances. What matters is that it addresses both the addiction and the underlying factors that led to use.
What Recovery and Healing Look Like
Once someone stops using meth and enters treatment, healing can begin. It is not instant. Existing sores will still take weeks or months to fully heal because the body has to go through the normal healing process without the interference of continued meth use, picking, and re-infection.
But the improvements start relatively quickly. Within days of stopping meth, the formication sensation usually decreases as dopamine levels begin to normalize and the nervous system starts to settle. Without the intense urge to pick, people stop creating new wounds. Within weeks, the body’s immune system begins to function better, white blood cells become more effective, and wound healing speeds up.
Over one to three months, existing active sores begin to scab over and close. Within three to six months, most of the open wounds have healed. Scarring will remain – deep pitted scars do not disappear – but they gradually become less red and less prominent. Skin tone often becomes more even as inflammation decreases.
In parallel, the person’s overall appearance often improves dramatically. Meth accelerates tooth decay, causes weight loss, creates sleep problems, and ages skin rapidly. As someone gets healthy in recovery, teeth get dental care, nutrition improves, sleep returns, and skin texture recovers somewhat. While meth scars may always be visible, the overall appearance can be dramatically different for someone actively engaged in recovery.
Recognizing Meth Sores in Someone You Love
If you are worried that someone close to you might be using meth, meth sores can be an important warning sign. A person who suddenly develops clusters of wounds on their face or arms, who claims to have a persistent rash or bug bites that do not respond to normal treatment, or who has visible scabs and scars on their face and hands may be using meth.
Other signs often go along with meth sores: rapid tooth decay (“meth mouth”), severe weight loss, skin that looks aged beyond the person’s years, sleep problems, agitation or paranoia, and unusual behavior like picking at imaginary things or feeling crawling sensations.
If you notice these signs in someone you care about, it is worth having a caring conversation about what is going on. Meth sores are often a sign that meth use has been heavy enough to cause physical damage, which means professional help is usually needed.
When to Seek Urgent Medical and Addiction Help
Anyone with meth sores that are very painful, hot to the touch, rapidly spreading, producing thick pus or greenish drainage, or accompanied by fever should seek emergency or urgent medical evaluation immediately. These can be signs of serious bacterial infection including MRSA or cellulitis, which can spread quickly and become life-threatening.
Even for non-urgent sores, it is worth seeing a healthcare provider to assess for infection risk and get proper wound care advice. At the same time, addressing the meth addiction should be the priority. Reaching out to a treatment program, calling a substance abuse helpline, or talking to a doctor about options for inpatient detox, PHP, or IOP can be the turning point that allows both healing of the skin and recovery of the whole person.
Frequently Asked Questions
Are meth sores contagious?
The sores themselves are not contagious. However, if they are infected with MRSA or other bacteria, those bacteria can potentially spread to other people through direct contact or shared items. It is important to keep infected sores covered and maintain good hygiene to prevent spreading infection to others.
Do meth sores go away completely after stopping meth?
Active sores will heal once meth use stops because the picking, poor healing, and re-infection cycle stops. However, deep scars from large infections or years of scarring often remain permanent or only fade slowly over time. Early intervention – stopping meth use sooner rather than later – can prevent the worst scarring.
Can dermatologists or plastic surgeons fix meth scars?
Dermatologists can sometimes improve the appearance of meth scars through treatments like laser resurfacing, chemical peels, or injectable fillers. But these are cosmetic treatments that work best after someone has been in stable recovery and the skin has finished healing and remodeling, which can take a year or longer. The primary goal should be stopping meth use and preventing new scars.
How do I talk to someone about their meth sores?
It is best to approach the conversation with genuine care rather than judgment. You might say something like, “I have noticed some sores on your skin and I am worried about you. I want to help. Have you thought about talking to a doctor or getting treatment?” Avoid being accusatory. Focus on concern for their health and wellbeing.
If You or Someone You Love Needs Help With Meth Addiction
Meth sores are a visible sign of how hard methamphetamine is on the body. They are also a sign that recovery is needed and possible. With proper addiction treatment with inpatient detox,people can stop using meth, allow their skin and body to heal, and rebuild their lives.
References
- NCBI Bookshelf – Methamphetamine (StatPearls)
- Neurologic Manifestations of Chronic Methamphetamine Abuse
- Methamphetamine Use and Methicillin-Resistant Staphylococcus aureus Skin Infections (CDC)
- Methamphetamine Alters the Antimicrobial Efficacy of Phagocytic Cells and Wound Healing
- Effects of Substance Use on Your Skin – American Addiction Centers
- SAMHSA – What Are Stimulants? Side Effects and Long-Term Effects