GHB has a strange dual existence in America. On one hand, it’s a legitimate FDA-approved prescription medicine used to treat narcolepsy under the brand name Xyrem. On the other, it’s a Schedule I controlled substance meaning it’s illegal to possess for any purpose other than the specific FDA-approved formulation with a reputation as a club drug linked to sexual assault and overdose deaths. Understanding what GHB actually is, what it does to the body, and why it’s so dangerous helps clarify why it carries such a serious legal and health status in the United States.
GHB at a Glance
- Street names: G, Gamma OH, Georgia Home Boy, Liquid Ecstasy, Liquid X
- Legal status (U.S.): Schedule I drug; illegal to possess without prescription. FDA-approved as Xyrem (Schedule III) for narcolepsy
- How it’s used: Ingested as liquid; takes effect in 15-30 minutes; effects last 3-6 hours
- Prevalence: 0.1% of Americans (161,000 people) used GHB in the past year; 0.6% (1.7 million) have used it lifetime
- Overdose risk: GHB has a steep dose-response curve; small increases in dose cause dramatically worse effects; no antidote exists
- Withdrawal: Severe and potentially life-threatening; can last up to 15 days
GHB (gamma-hydroxybutyrate) is a naturally occurring chemical in the human brain, but when concentrated and used recreationally, it becomes a powerful central nervous system depressant. Chemically, it’s a four-carbon compound that crosses the blood-brain barrier easily, meaning it reaches the brain quickly and creates profound effects.
The FDA-approved version is sodium oxybate, sold as Xyrem, which is prescribed at specific doses to help people with narcolepsy manage excessive daytime sleepiness and muscle weakness (cataplexy). When people talk about “GHB” on the street, they’re almost always referring to illicit, unregulated versions manufactured in clandestine labs or diverted from pharmaceutical sources.
Street GHB comes as a clear, colorless, odorless liquid with a salty taste. It’s often sold in small vials or bottles, sometimes labeled as “research chemical” or other misleading names. Because it has no color or distinct taste, it can be mixed into drinks without the person knowing, which is why it earned the nickname “date rape drug”.
How GHB Works?
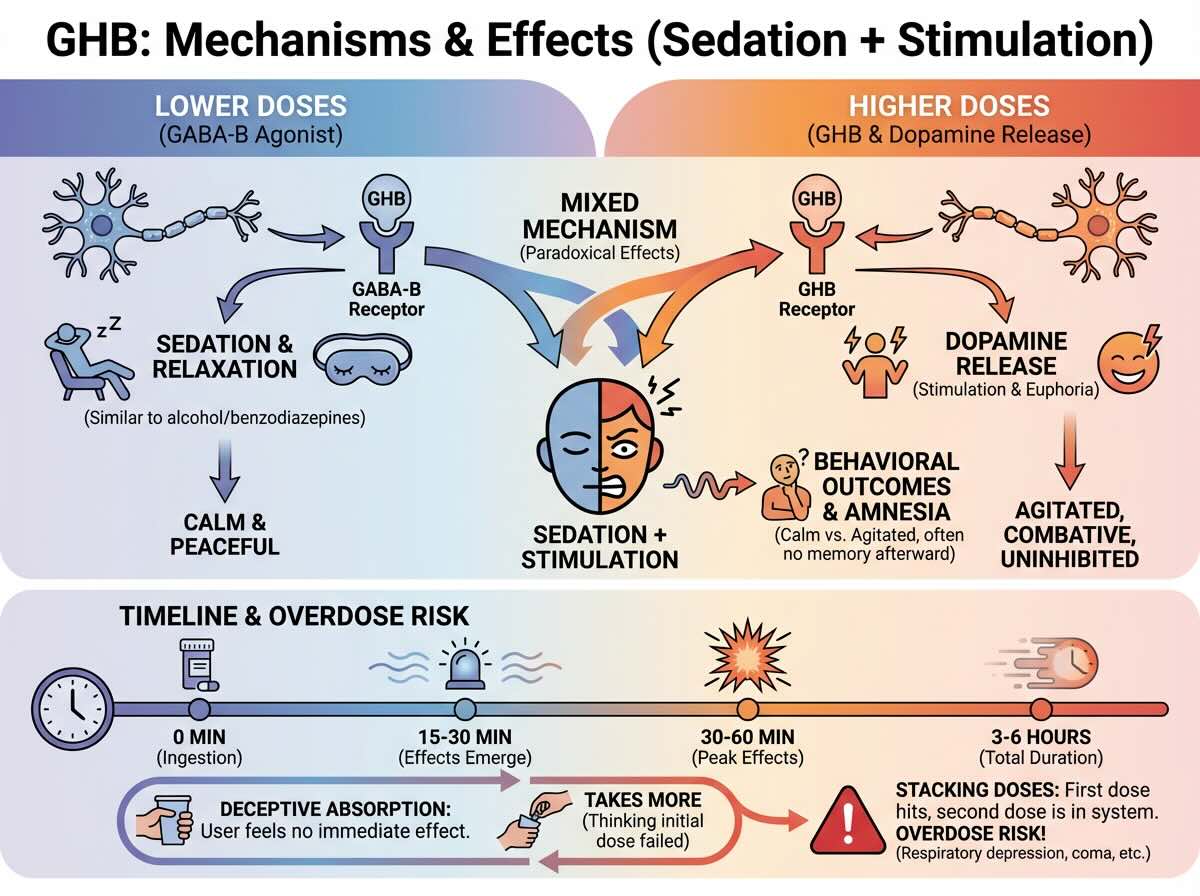
GHB works primarily through two mechanisms. At lower doses, it acts as a GABA-B receptor agonist, creating sedation and relaxation similar to alcohol or benzodiazepines. At higher doses, it also activates its own receptor (the GHB receptor), which paradoxically increases dopamine release, creating stimulation and euphoria alongside sedation.
This mixed mechanism, sedation plus stimulation, explains why GHB users sometimes appear calm and peaceful, while other times they become agitated, combative, or sexually uninhibited, often without remembering their behavior afterward.
Effects typically emerge within 15-30 minutes of ingestion, peak around 30-60 minutes, and last 3-6 hours total. The quick absorption and elimination make GHB deceptive: users don’t feel effects immediately, so they may take more, thinking the initial dose didn’t work. By the time the first dose hits, the second dose is already in the system, creating overdose risk.
GHB users in the United States tend to be young, well-educated, and fairly evenly split between men and women. However, it’s used at disproportionately high rates within LGBTQ+ communities, particularly gay and bisexual men, and in “chemsex” contexts where it’s used alongside other drugs for sexual enhancement.
GHB also concentrates in nightclub, rave, and festival settings, where users seek its euphoric and disinhibiting effects. Some bodybuilders and fitness enthusiasts have historically used GHB for its reported muscle-building and fat-loss properties, though these effects are unproven.
Common reasons people use GHB include euphoria and disinhibition (social confidence, reduced anxiety), sexual enhancement, sleep promotion, and perceived muscle-building. Because GHB is tasteless, colorless, and odorless, it can be added to drinks without consent, which has made it a weapon in drug-facilitated sexual assault.
The History of GHB in the United States
GHB’s journey in America tells a story of a substance that moved from legitimate pharmaceutical development to recreational drug to Schedule I controlled substance in less than two decades.
The Evolution of GHB: From Medicine to Regulation
1874 – 1980s: Discovery & The Fitness Boom
GHB was first synthesized in 1874 by a French chemist, but it remained obscure until the 1960s when Soviet researchers identified its sedative and anesthetic properties.
The 1990s: Nightclubs and Public Alarm
By the late ’80s and early ’90s, GHB transitioned from gyms to the rave scene. Known as “Liquid Ecstasy,” it was prized for its euphoric and disinhibiting effects.
“The turning point came in the mid-1990s when GHB became widely known as a ‘date rape drug’ due to its tasteless, colorless nature and its ability to cause memory loss.”
2000 – 2002: Federal Regulation & The Dual-Schedule
In 2000, Congress passed the Hillory J. Farias and Samantha Reid Date-Rape Prevention Act, creating a unique legal paradox:
| Category | Legal Status | Context |
|---|---|---|
| Recreational GHB | Schedule I | Illegal to possess; no accepted medical use. |
| Sodium Oxybate (Xyrem) | Schedule III | FDA-approved in 2002 for narcolepsy/cataplexy. |
2010 – Present: The Modern Resurgence
While use declined sharply after the 2000 ban, a second wave of popularity began around 2010, particularly within LGBTQ+ communities and “chemsex” contexts.
- 2008: Poison Control calls bottomed out at 448.
- 2020: Poison Control calls rose to 776 and continue to climb.
Factors Driving Resurgence:
- Digital Access: Social media and underground channels allow for discreet purchasing.
- Legal Grey Areas: Industrial analogues like GBL and BD complicate law enforcement.
- Private Settings: A shift from public nightclubs to private residences and online communities.
Today, nearly 25 years after the Hillory J. Farias Act, GHB remains Schedule I and illegal to possess recreationally in the United States. However, it continues to circulate in underground markets, particularly in urban areas and within specific communities. The contrast between GHB’s strict legal status and its persistent availability illustrates the challenge of controlling drugs that have both medical utility and high abuse potential.
GHB Overdose: The Narrow Safety Margin
GHB’s primary danger lies in its steep dose-response curve, meaning small increases in dose produce dramatically worse effects. There’s a narrow gap between a dose someone perceives as “safe” and a dose that causes coma or death.
Several factors create overdose risk even for experienced users: individual tolerance varies widely between people and changes day-to-day; street GHB varies dramatically in concentration with no way to know actual dosing; polydrug interactions with alcohol, benzodiazepines, opioids, or other CNS depressants increase toxicity exponentially (alcohol is present in 76% of GHB-related emergency visits); and redosing before effects appear because GHB takes 15-30 minutes to work.
The reality most people don’t understand: there is no antidote for GHB overdose. Once someone has overdosed, the only treatment is aggressive supportive care in an intensive care unit, including mechanical ventilation if breathing stops, seizure medications, and continuous monitoring until the drug leaves the system.
A study of people with GHB dependence found that between 25-69% reported experiencing GHB-induced coma at some point in their using history. Coma from GHB is not uncommon, it’s a common risk of the drug itself.
Overdose Symptoms and What Happens
The classic pattern of GHB overdose is a sudden loss of consciousness followed by an abrupt awakening within hours. However, at higher doses, the overdose can be more severe and include:
- Respiratory depression or apnea (stopped breathing)
- Seizures
- Bradycardia (dangerously slow heart rate)
- Hypotension (low blood pressure)
- Vomiting and aspiration (choking on vomit)
- Hypothermia (dangerously low body temperature)
- Coma lasting hours or days
- Death
People can overdose without intending to because the difference between an effective dose and an overdose is small and unpredictable. A dose that causes mild euphoria one day might cause coma the next day depending on tolerance, food in the stomach, body weight, and other variables. Additionally, street GHB purity varies widely, what someone believes is a standard dose might actually be 2-3 times stronger.
Emergency room staff often struggle to treat GHB overdose because the drug works in a window: at very high doses, people are unconscious and unresponsive, but they typically wake up on their own within 4-8 hours as their body metabolizes the drug. If respiratory depression occurs, mechanical ventilation is necessary. If seizures occur, anticonvulsants are needed. But there’s no drug that reverses or speeds up GHB elimination.
Because GHB itself is strictly controlled, clandestine manufacturers often produce two GHB “analogues” chemicals that convert to GHB once inside the body: GBL (gamma-butyrolactone), sold as “ink cartridge cleaner,” “stain remover,” or “nail enamel remover” for approximately $100 per bottle, and 1,4-BD (1,4-butanediol), sold under similar “cleaning product” labels.
Both rapidly convert to GHB once ingested, producing identical effects and overdose risks. From a user’s perspective, GBL and BD are functionally identical to GHB same high, same risks, same potential for overdose but easier to obtain because they’re marketed as industrial chemicals.
Is GHB Addictive? The Dependence Cycle
Yes, GHB is highly addictive. Regular use leads to both psychological dependence (craving, compulsive use) and physical dependence (withdrawal symptoms when stopping).
Addiction develops relatively quickly with GHB, often within weeks to months of regular use. Users report that the drug’s euphoric and disinhibiting effects create strong craving, particularly in social or sexual contexts where GHB use becomes tied to pleasure and connection.
Physical dependence develops because the brain adapts to constant GHB presence by downregulating receptors and altering neurotransmitter balance. When GHB is removed, the brain is left in a state of extreme imbalance, producing withdrawal symptoms.
The cycle is self-perpetuating: regular users redose frequently (sometimes every 2-4 hours while awake) to maintain euphoria and avoid withdrawal. This redosing pattern, combined with the narrow safety margin, creates extreme overdose risk for people with established dependence.
Users with GHB dependence often describe it as more difficult to quit than heroin or alcohol because withdrawal is so severe and the craving so intense.
GHB Withdrawal: Why Quitting Requires Medical Help
The withdrawal syndrome from GHB is unique and dangerous. Unlike some withdrawal syndromes that are acutely uncomfortable but not medically dangerous, GHB withdrawal can include seizures and delirium that require ICU-level care.
Withdrawal symptoms typically include tremors, agitation, anxiety, increased heart rate and blood pressure, insomnia, and hallucinations. In severe cases, seizures and delirium (confusion, disorientation, psychotic symptoms) occur. These complications can be life-threatening.
The critical point: GHB withdrawal can last up to 15 days and requires medical supervision in an intensive care setting. The timeline typically follows this pattern:
- Hours 6-12 after last use: Anxiety, tremors, insomnia begin
- Hours 12-24: Agitation, hallucinations, vital sign increases
- Days 2-3: Peak severity; seizures and delirium most likely
- Days 4-15: Gradual improvement with medical support
GHB Withdrawal Timeline
| Timeframe | Symptoms & Progression |
|---|---|
| Hours 6-12 | Anxiety, tremors, and insomnia begin. |
| Hours 12-24 | Agitation, hallucinations, and vital sign increases. |
| Days 2-3 | Peak severity: Seizures and delirium most likely to occur. |
| Days 4-15 | Gradual improvement with continuous medical support. |
Note: GHB withdrawal requires medical supervision in an intensive care setting due to life-threatening complications.
Stopping GHB abruptly can be more dangerous than continuing use, which is why medical detoxification is essential rather than trying to quit “cold turkey”. Medical detoxification typically involves benzodiazepines to manage agitation and prevent seizures, anticonvulsants if seizure risk is high, and continuous monitoring of vital signs.
With proper medical supervision, people successfully withdraw from GHB and enter recovery. But it requires specialized care from medical professionals experienced with this specific withdrawal syndrome.
GHB use prevalence in the United States shows concerning trends: 1.7 million Americans (0.6% of the population age 12+) have used GHB at least once, while 161,000 Americans (0.1%) used GHB in the past year. Poison Control received 563 case mentions of GHB in 2023, with 97 resulting in major medical outcomes. GHB mentions to Poison Control peaked in 2002 (1,386 calls), dropped to 448 in 2008, then rose again to 776 by 2020, indicating a significant resurgence in use.
In the United States, GHB carries one of the strictest legal classifications: Schedule I (illegal to possess, manufacture, or distribute; no accepted medical use except for FDA-approved Xyrem, which is Schedule III). Possession without a prescription is a felony; distribution carries even more severe penalties. Possession for personal use can result in a criminal record, fines up to $250,000, and federal imprisonment. Distribution carries up to 20 years in prison.
GHB occupies a unique place among recreational drugs. It’s not the most prevalent, but it’s among the most dangerous because of its narrow safety margin, unpredictability, lack of an antidote, and highly addictive properties. If you’re using GHB, becoming dependent, or concerned about someone who is, the most important thing to understand is that medical help exists and makes a real difference. Detoxification is complex and dangerous, but with proper medical supervision, people recover successfully.
Official Resources & References
- Drug Enforcement Administration (DEA):
GHB Drug Fact Sheet & Statistical Update - National Institute on Drug Abuse (NIDA):
GHB Research Report - Food and Drug Administration (FDA):
Xyrem (Sodium Oxybate) Prescribing & Safety Information - SAMHSA:
2024 National Survey on Drug Use and Health (NSDUH) - Congress.gov:
H.R.2130 – Hillory J. Farias and Samantha Reid Date-Rape Prevention Act - America’s Poison Centers:
2023-2024 Annual Report of the National Poison Data System