When someone is ready to address an alcohol or drug addiction, one of the first big choices is between inpatient vs outpatient care. Both can support long term recovery, but they feel very different day to day, and national data show that people often move between these levels of care rather than using only one.
Key Points
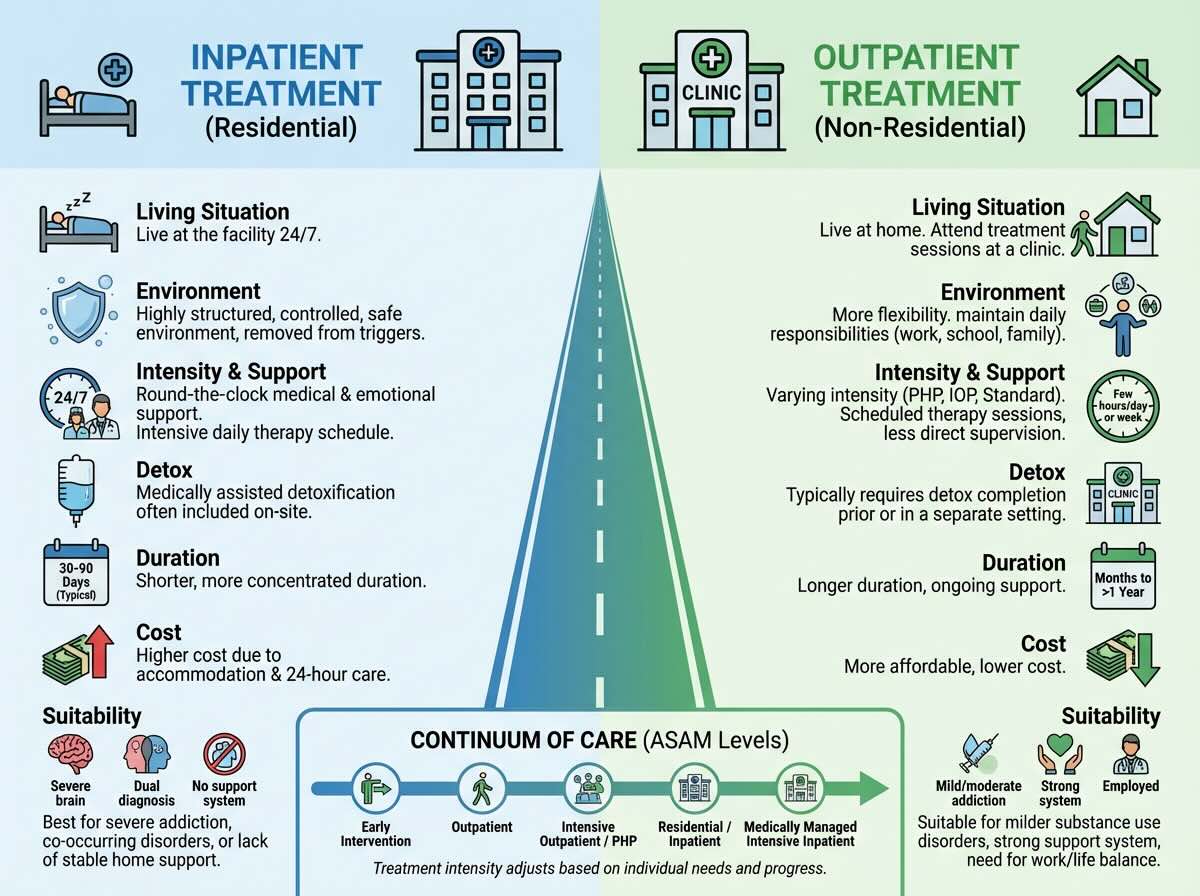
- Inpatient care: You live at the facility full time with 24 hour medical and clinical support. This level of care is especially important when detox is medically risky, cravings are intense, or home is not a safe place to stabilize.
- Outpatient care: You live at home and attend therapy on a set schedule while you keep your usual responsibilities. Outpatient can range from a few hours per week to several days per week in more intensive formats.
- Outpatient is the most common setting: Recent federal facility surveys show that well over 80 percent of substance use treatment programs in the United States offer some form of outpatient care, while a smaller share provide residential or hospital based inpatient services.
- Need is widespread: National surveys estimate that tens of millions of Americans have a substance use disorder in a given year, but only a fraction receive specialty treatment. That gap is one reason why flexible outpatient options and step down care have grown so quickly.
Inpatient vs Outpatient – Key Differences
One way to think about inpatient versus outpatient is to picture how much of your time is wrapped in treatment. Inpatient or residential care is like pressing pause on normal life so that nearly every hour of the day supports recovery, including sleep, meals, groups, and downtime. Outpatient care weaves treatment into your existing routine so you can keep working, going to school, or caring for family while you address addiction.
Large national datasets that track treatment episodes emphasize that the better question is not “which is better overall” but “which is the best match for this person right now.” Someone with a long history of relapse, unstable housing, or serious withdrawal risks usually needs more structure at the beginning. Someone with mild to moderate symptoms, a stable home, and strong support may do well starting in an intensive outpatient or standard outpatient program.
| Aspect | Inpatient Treatment | Outpatient Treatment |
|---|---|---|
| Where you live | On site at the facility, usually 30–90 days at a time | At home, commuting to sessions |
| Support level | 24 hour access to medical and clinical staff, especially around detox and early stabilization | Support during scheduled visits, with check ins between sessions in some programs |
| Treatment intensity | Multiple groups, individual counseling, and recovery activities most days | From weekly sessions up to several days per week in intensive outpatient formats |
| Daily responsibilities | Work and school usually paused so you can focus on treatment | Work, school, and caregiving continue alongside treatment |
| Environment | Substance free, structured environment with fewer immediate triggers | Ongoing exposure to home and community triggers, which can be both a risk and a chance to practice skills |
| Typical next step | Step down to intensive outpatient or standard outpatient after discharge | Continue as maintenance care, or step up to a higher level if symptoms worsen |
When Inpatient Care Makes Sense
Inpatient care is often recommended when safety is the first priority. Alcohol, benzodiazepine, and some opioid withdrawals can be medically complicated, and having a team monitor blood pressure, heart rate, and other vital signs around the clock lowers the risk of serious events. Hospital based and residential programs can also manage medications that ease withdrawal and cravings in a controlled setting.
People who have tried to quit many times on their own, or have cycled in and out of shorter outpatient efforts, often benefit from the “reset” that inpatient provides. Being physically removed from people, places, and routines linked to substance use gives the brain and body time to settle. Inside that protected space, there is room for structured therapies, family sessions, and planning for what life will look like after discharge instead of simply reacting to daily crises.
National treatment guidance highlights that effective inpatient programs go beyond detox. They weave in evidence based therapies, such as cognitive behavioral approaches and motivational strategies, and screen for mental health conditions like depression, anxiety, and trauma, which are common among people in treatment. Addressing those issues under one roof can make the transition to lower levels of care smoother and more sustainable.
Why Outpatient Is So Common
Outpatient care is the most common treatment setting in the U.S. partly because it is flexible and scalable. Programs can schedule sessions across the week, offer evening or daytime groups, and tailor intensity without needing large numbers of beds. That flexibility helps reach more of the millions of people who meet criteria for a substance use disorder each year but live far from a hospital or residential facility.
For many people, the biggest strength of outpatient care is the chance to practice recovery skills in real time. You might learn a craving management technique in group, try it that evening when you drive past an old bar or dealer’s neighborhood, and then come back the next day to talk about what helped and where you struggled. That immediate feedback loop can be powerful when your home is stable and your support system is engaged.
Outpatient also plays a major role as step down care after more intensive treatment. National principles of effective treatment emphasize that recovery is a long term process, not a single event. Moving from inpatient to intensive outpatient to weekly counseling over months, rather than ending all contact at discharge, is one way people maintain gains and reduce the risk of relapse.
Choosing Between Inpatient and Outpatient
When you are trying to decide where to start, it can help to ask three questions. First, how medically risky is it for you to stop using. Second, what happens when you try to stop while living at home. Third, who and what are around you day to day. If you have had seizures or severe withdrawal in the past, if you relapse very quickly at home, or if the people you live with are still using, that usually points toward starting in a higher level of care.
On the other hand, if your withdrawal risks are low, your home is substance free, and you have people who support your recovery, starting in outpatient care can be a realistic and respectful choice. You still get structured help, but you do not have to step away from all of your roles and responsibilities. You can also move up to a more intensive program later if it turns out that early recovery is harder than expected.
What Drives Better Outcomes
Across large national treatment datasets, one theme shows up repeatedly: time in treatment and ongoing connection matter. People who stay engaged for longer periods, who complete at least several months of combined inpatient and outpatient care, and who continue with some form of follow up support tend to have better long term outcomes than those who leave early or disappear between levels of care.
Research based guidance also notes that addressing the whole person is key. The most effective programs do not just count days without substances. They ask about mental health, physical health, housing, employment, legal stress, and family relationships, then build a plan around those realities. When these pieces are coordinated across inpatient and outpatient settings, recovery has a stronger foundation.
Why Choose Inpatient Care at Still Detox
For many people, the safest and most comfortable way to start recovery is in a structured inpatient setting. At Still Detox in Boca Raton, inpatient treatment combines 24 hour medical monitoring with a calming, private environment so you are not trying to manage withdrawal or early cravings on your own.
Care is medically supervised from the moment you arrive, which means a licensed team is watching your vital signs, adjusting medications when appropriate, and checking in on how you are feeling physically and emotionally. This level of attention can lower the risk of complications from alcohol, opioid, or sedative withdrawal and makes it easier to focus on the next steps in your treatment plan, not just on getting through the night.
Beyond the medical piece, inpatient care at Still Detox gives you space away from daily pressures and triggers. You are surrounded by staff who understand addiction, peers who are working toward the same goal, and a schedule that includes therapy, rest, and time to reset. For many people and families, that combination of safety, privacy, and structure is what finally makes change feel possible.
FAQ
Is outpatient always less effective than inpatient?
No. Both inpatient and outpatient can be effective when the level of care matches your needs and you stay in treatment long enough to build new routines and supports.
How many programs offer inpatient care?
National facility data show that most providers offer at least one form of outpatient treatment, while a smaller share provide residential or hospital based inpatient programs. That is one reason many people start in outpatient care or step down into it after a residential stay.
How long should treatment last overall?
Guidance from national research agencies suggests that, for many people, less than about 90 days of total treatment is often not enough, whether that time is in residential, inpatient, or outpatient care. Longer engagement and planned step downs are linked with better outcomes on average.
References
- Substance Abuse and Mental Health Services Administration (SAMHSA) – National substance use and treatment data
- National Institute on Drug Abuse (NIDA) – Principles of Drug Addiction Treatment: A Research Based Guide
- KFF – A Look at Substance Use and Mental Health Treatment Facilities Across the U.S.
- SAMHSA – Treatment Episode Data Set (TEDS) 2023