Black tar heroin is a crude, low-purity form of heroin named for its dark, sticky, tar-like appearance. It is produced primarily in Mexico and is the dominant form of illicit heroin distributed west of the Mississippi River in the United States. Unlike white or brown powder heroin, black tar heroin is a gummy, dark brown to black substance that resembles roofing tar or hardened molasses.
It is the same drug class as powder heroin but manufactured through a faster, less refined process that leaves significantly more chemical impurities behind. Those impurities do not reduce its danger. They add to it, introducing unique infection risks and overdose variables that powder heroin does not carry at the same level.
If someone you know is using black tar heroin, understanding exactly what it is, how it works, and why it causes physical dependence so rapidly is the critical first step toward getting them the right help before an overdose or a life-threatening infection occurs.
Key Highlights
- Black tar heroin is a Schedule I controlled substance with no accepted medical use, produced primarily in Mexico through an incomplete acetylation process that leaves the final product 25 to 30% pure at best (DEA, 2020).
- According to the 2020 National Survey on Drug Use and Health, 902,000 people aged 12 and older used heroin in the previous year, and 691,000 met the clinical criteria for heroin use disorder (SAMHSA, 2021).
- Black tar heroin carries a uniquely elevated risk of wound botulism, a rare but potentially fatal bacterial infection. Between 2001 and 2016, 82% of all wound botulism cases reported to the CDC occurred in California, where black tar heroin is the predominant street form of the drug (CDC, 2019).
- Studies report that approximately 80% of people who use heroin first misused a prescription opioid, highlighting the direct pipeline from untreated opioid dependence to illicit heroin use (AddictionCenter, 2024).
- Heroin use disorder is a treatable medical condition. FDA-approved medications combined with behavioral therapy produce the strongest outcomes for lasting recovery.
What Is Black Tar Heroin? Definition and Chemical Identity
Heroin is a semisynthetic opioid derived from morphine, which is extracted from the opium poppy plant. All forms of heroin share the same base chemical structure, diacetylmorphine, but differ significantly in purity, appearance, and manufacturing process.
Black tar heroin is produced through an incomplete acetylation of morphine, a shorter and cheaper production method that skips the purification steps required to make powder heroin. The result is a product with extremely variable purity, typically between 25 and 30% actual heroin content, with the rest made up of processing byproducts, cutting agents, and contaminants picked up during transport and handling.
The DEA classifies heroin as a Schedule I controlled substance, meaning it has no currently accepted medical use and carries the highest potential for abuse and physical dependence in the federal drug scheduling system. Any possession or distribution of black tar heroin is a federal criminal offense.
Understanding the full scope of the opioid epidemic in 2025 helps explain why black tar heroin remains so deeply entrenched in communities across the western United States despite decades of enforcement efforts.
What Does Black Tar Heroin Look Like?
Black tar heroin is visually distinct from all other forms of heroin, which is one of the easiest ways to identify it. For a full visual comparison of heroin forms, see our guide to what does heroin look like.
- Color: Dark brown to jet black. Occasionally a very dark reddish-brown depending on cutting agents used in production.
- Texture: Sticky, gummy, and tacky in its natural state, similar to roofing tar or thick molasses. Can harden into a rock-like chunk when cooled or dried.
- Consistency: Ranges from soft and pliable to hard and brittle. Users often soften it between their fingers or with heat before use.
- Smell: Strong vinegar-like odor, more pungent than powder heroin, caused by residual acetic acid left from incomplete manufacturing.
Black Tar Heroin vs. Powder Heroin
| Feature | Black Tar Heroin | Powder Heroin |
|---|---|---|
| Appearance | Dark brown to black, sticky or hard | White to brown, fine powder |
| Purity | 25 to 30% | Up to 80% or higher |
| Primary origin | Mexico | Afghanistan, South America |
| Common US region | West of the Mississippi | East Coast cities |
| Can be snorted raw | No (must be dried first) | Yes |
| Wound botulism risk | Significantly elevated | Much lower |
| Street price | Lower | Higher |
| Fentanyl adulteration | Increasingly common | Extremely common |
Black Tar Heroin Street Names and Slang
Black tar heroin circulates under several regional street names. Knowing this slang is important for parents, educators, and anyone trying to identify whether someone they care about is using the drug. For a complete list of heroin terminology, visit our page on heroin street names, slang, and nicknames.
- Black tar
- Mexican mud
- Mexican black tar
- Black pearl
- Black eagle
- Chiva
- Black stuff
- Tar
- Mud
- Dragon (when smoked)
How Is Black Tar Heroin Used?
Black tar heroin in its natural gummy form cannot be snorted without being dried and crushed first. Users must dissolve or otherwise prepare it before administration. The methods most associated with black tar heroin are:
- Injecting intravenously (IV): Users dissolve the drug in water, heat it in a spoon, and inject it directly into a vein. This is the fastest method, with effects felt within seconds. It carries the highest risk of collapsed veins, abscesses, HIV, hepatitis C, and wound botulism.
- Skin popping (subcutaneous injection): Injecting under the skin rather than into a vein. Creates the anaerobic wound environment most associated with wound botulism and gas gangrene in black tar heroin users specifically.
- Muscling (intramuscular injection): Injecting into muscle tissue. Carries the same elevated infection risks as skin popping.
- Smoking (chasing the dragon): The drug is placed on aluminum foil and heated from below while the vapor is inhaled through a tube. More common with black tar than with powder heroin because it requires no dissolving.
- Snorting: Less common with black tar due to texture but possible after drying and crushing. Damages nasal tissue progressively. For the specific risks of this method, see our resource on snorting heroin.
Because black tar heroin requires dissolving and heating before injection, users often add acidic substances including lemon juice or vitamin C powder to help it break down. This process does not remove bacterial contamination and can itself introduce additional pathogens into the solution.
What Does Black Tar Heroin Do to the Brain and Body?
Black tar heroin works identically to other forms of heroin at the neurological level. Once it enters the bloodstream it crosses the blood-brain barrier and binds to mu-opioid receptors throughout the brain and central nervous system. This binding triggers a massive dopamine release and shuts down pain signaling, producing the characteristic heroin rush.
Short-Term Effects
- Intense euphoria and a warm, full-body rush within seconds of IV injection
- Drowsiness, heavy limbs, and clouded thinking
- Nausea and vomiting, especially in newer users
- Severe itching and skin flushing
- Slowed breathing and reduced heart rate
- Pinpoint pupils regardless of lighting conditions
- Dry mouth and slurred speech
- Nodding, alternating between consciousness and semi-consciousness
Long-Term Effects of Chronic Use
Repeated heroin use causes measurable structural and neurochemical changes to the brain. Research has shown deterioration of white matter in the brain among long-term heroin users, impairing decision-making, behavioral regulation, and stress response capacity.
- Tolerance developing rapidly, requiring larger and larger doses
- Physical dependence, where the body cannot function normally without heroin
- Opioid use disorder (heroin use disorder), the DSM-5 clinical diagnosis for addiction
- Collapsed and scarred veins from repeated injection
- Skin abscesses, open sores, and tissue death at injection sites
- Endocarditis, infection of the heart lining and valves
- Elevated risk of HIV and hepatitis C from shared needles
- Liver and kidney damage
- Chronic constipation and gastrointestinal damage
- Pneumonia and respiratory complications
- Severe depression and anxiety between doses
- Cognitive decline including memory loss and impaired judgment
The full range of opioid addiction symptoms and effects explains how heroin use disorder progresses across each organ system over time.
Unique Dangers of Black Tar Heroin
Beyond the standard heroin risks shared with all forms of the drug, black tar heroin carries specific dangers rooted in its impurity and production environment.
Wound Botulism
Wound botulism is a rare but potentially fatal bacterial infection caused by Clostridium botulinum, a bacterium that produces a neurotoxin capable of causing descending paralysis and death from respiratory failure. Black tar heroin carries a dramatically higher botulism risk than powder heroin because its production in unsanitary conditions, transport hidden inside car tires or other contaminated containers, and crude preparation methods allow Clostridium botulinum spores to survive and contaminate the supply.
Critically, cooking black tar heroin before injection does not destroy these spores. They survive high heat and can germinate in wound tissue, particularly when the drug is injected under the skin or into muscle rather than directly into a vein.
Between 2001 and 2016, the CDC received reports of 353 wound botulism cases in the United States. Of those, 291 cases (82%) came from California, where black tar heroin is the dominant street drug (CDC, 2019). In 2017, 17 of 19 laboratory-confirmed wound botulism cases in the US were linked to injection drug use (PMC, 2021).
Wound botulism symptoms from black tar heroin include:
- Drooping eyelids and double or blurred vision
- Difficulty speaking or swallowing
- Progressive muscle weakness moving downward from the face
- Shortness of breath and difficulty breathing
- Arm and leg weakness with reduced reflexes
Symptoms typically appear several days after injection, causing dangerous diagnostic delays. Emergency treatment requires botulism antitoxin and in severe cases surgical debridement. Without prompt treatment, wound botulism can be fatal.
Gas Gangrene
Gas gangrene is caused by Clostridium perfringens bacteria entering the bloodstream through injection sites. It is a rapidly progressing, life-threatening soft tissue infection that can destroy muscle and skin tissue within hours. Like botulism, it is specifically associated with black tar heroin injection, particularly skin popping and muscling, and is essentially not seen with powder heroin use.
Fentanyl Contamination
Fentanyl contamination of black tar heroin has grown sharply in recent years and is now a primary driver of heroin-related overdose deaths. Fentanyl is 50 to 100 times more potent than morphine and is added to heroin supplies because it is cheaper to produce and dramatically increases perceived potency.
Users cannot detect fentanyl in black tar heroin by sight, smell, or feel. A batch that appears and feels identical to previous purchases may contain a lethal concentration of fentanyl. In one study, nearly 3 in 5 people exposed to fentanyl-contaminated heroin were unaware of the contamination beforehand. The danger of counterfeit pills and fentanyl contamination extends across all illicit opioid markets, including black tar heroin.
Fentanyl test strips can detect fentanyl presence in a drug supply and are available through harm reduction programs in many states. A negative result does not eliminate overdose risk from heroin alone.
Signs of Black Tar Heroin Addiction
Heroin addiction is clinically diagnosed as opioid use disorder (OUD) under DSM-5 criteria. The brain adapts to constant heroin exposure by reducing its natural opioid receptor activity, making normal function impossible without the drug. This is the neurological foundation of physical dependence.
Signs that someone has developed opioid use disorder from black tar heroin include:
- Using heroin in larger amounts or for longer periods than intended
- Repeated failed attempts to cut down or stop
- Spending significant time obtaining, using, or recovering from heroin
- Intense cravings between doses
- Neglecting work, school, or family responsibilities because of heroin use
- Continuing to use despite clear physical harm or relationship breakdown
- Developing tolerance, requiring increasingly larger doses for the same effect
- Experiencing withdrawal symptoms when stopping or reducing use
- Wearing long sleeves in warm weather to conceal track marks or injection sites
- Social withdrawal and rapidly declining personal hygiene
Physical signs specific to black tar heroin use include needle punctures, bruising, or hardened tissue at injection sites, skin abscesses or open sores from skin popping, and the presence of syringes, spoons, lighters, and aluminum foil among belongings. A detailed breakdown of behavioral warning signs is available in our guide to heroin addiction symptoms and effects.
Black Tar Heroin Withdrawal Symptoms and Timeline
Heroin withdrawal is physically intense and begins as the drug clears the system and suppressed opioid receptors reassert activity without chemical support. While rarely fatal on its own, heroin withdrawal significantly increases relapse risk and is the primary reason people cannot sustain abstinence without clinical support.
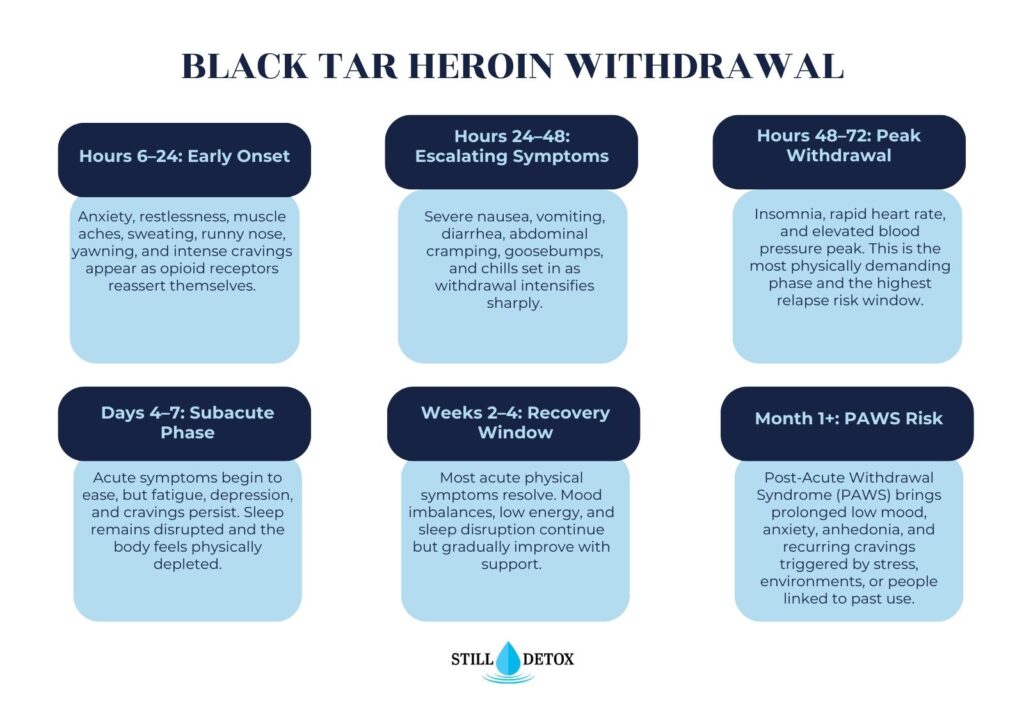
- Early withdrawal (hours 6 to 24 after last dose): Anxiety, restlessness, muscle aches, sweating, runny nose, yawning, and intense cravings as the body begins signaling urgent need for the drug.
- Peak withdrawal (hours 24 to 72): Severe nausea, vomiting, diarrhea, abdominal cramping, goosebumps, chills, insomnia, elevated heart rate, and high blood pressure. This is the most physically demanding phase.
- Subacute phase (days 4 to 7): Symptoms begin to ease but fatigue, depression, and cravings persist. Sleep remains disrupted and the person feels physically depleted.
- Post-acute withdrawal syndrome or PAWS (weeks to months): Prolonged low mood, difficulty experiencing pleasure (anhedonia), anxiety, and recurring cravings triggered by stress, environments, or people associated with prior use.
Attempting to detox from heroin at home is dangerous. Dehydration from vomiting and diarrhea can become medically serious. Relapse during withdrawal carries an extremely high overdose risk because tolerance drops rapidly during abstinence and a previously manageable dose can now be fatal. Our heroin withdrawal timeline resource provides a phase-by-phase breakdown of what to expect at every stage.
How Long Does Black Tar Heroin Stay in Your System?
Detection windows depend on the test type, dose, frequency of use, metabolic rate, body composition, and hydration. For a complete pharmacokinetic breakdown, see our guide to how long heroin stays in your system.
- Urine: Detectable for 1 to 4 days. The most commonly used test type. Chronic heavy users test at the longer end of this range.
- Blood: Detectable for up to 24 hours. Used after accidents, arrests, or in clinical settings where recent use needs quick confirmation.
- Saliva: Detectable for 1 to 3 days. Commonly used for roadside drug testing because of its rapid administration.
- Hair follicle: Detectable for up to 90 days. The most sensitive test for long-term or repeated use patterns.
Black Tar Heroin Overdose: Warning Signs and What to Do
A heroin overdose is a life-threatening emergency. It occurs when the amount of heroin overwhelms the respiratory system, causing breathing to slow or stop completely. Fentanyl contamination makes overdose thresholds completely unpredictable, even for experienced users with established tolerance.
Warning signs of a black tar heroin overdose:
- Extremely slow, shallow, or stopped breathing
- Blue or grayish lips, fingertips, or skin (cyanosis)
- Completely unresponsive or impossible to wake
- Gurgling or choking sounds
- Limp body with no muscle tone
- Pinpoint pupils even in very low light
- Pale, cold, and clammy skin
Call 911 immediately. Administer naloxone (Narcan) if available. Because fentanyl-contaminated black tar heroin is significantly more potent than standard heroin, multiple doses of naloxone may be required to reverse the overdose. All 50 US states have Good Samaritan laws providing legal protection for people who call for help during an overdose. Place the person on their side in the recovery position to prevent choking on vomit. Stay with them until emergency services arrive.
Black Tar Heroin vs. Heroin: Is Black Tar More Dangerous?
Black tar heroin and powder heroin are chemically identical in their active compound but differ significantly in purity, preparation, and risk profile. For a detailed comparison of heroin and methamphetamine, two of the most commonly co-used illicit opioids, see our heroin vs. meth comparison.
In practice, black tar heroin is considered more dangerous than powder heroin in several specific ways:
- Its impurities and production environment make it uniquely prone to wound botulism and gas gangrene contamination
- Its sticky consistency makes it harder to dose accurately, increasing overdose risk
- Skin popping and muscling, more common with black tar, create the exact infection conditions that favor bacterial growth
- Its lower cost and regional availability make it accessible in communities with fewer harm reduction resources
Both forms carry extreme addiction potential, high overdose risk, and the same capacity to cause opioid use disorder. Neither form is safer than the other in any absolute sense.
Treatment for Black Tar Heroin Addiction at Still Detox
Opioid use disorder is a treatable medical condition. FDA-approved medications combined with evidence-based behavioral therapy give people the best chance of achieving and sustaining lasting recovery from black tar heroin addiction. Still Detox provides medically supervised detox and residential treatment at our Boca Raton, Florida facility.
Our approach to heroin addiction treatment includes:
- Medical detox: 24-hour nursing and physician supervision through the acute withdrawal phase. Medications including buprenorphine and methadone ease withdrawal symptoms and reduce early relapse risk during the most vulnerable days of recovery. Our detoxification program is structured around clinical safety and individual comfort.
- Medication-assisted treatment (MAT): FDA-approved medications for opioid use disorder block cravings, reduce withdrawal severity, and lower overdose risk. Our medication-assisted treatment FAQ explains every available option in plain language.
- Dual diagnosis care: Many people who use black tar heroin have underlying depression, anxiety, trauma, or PTSD that preceded or worsened during addiction. Our dual diagnosis program treats both conditions simultaneously, which consistently produces better long-term outcomes than treating either condition alone.
- Cognitive behavioral therapy (CBT): Targets the thought patterns, emotional triggers, and high-risk situations that maintain opioid use. CBT combined with MAT represents the strongest clinical evidence base for opioid use disorder treatment.
- Long-term residential care: For those who need extended structure beyond initial detox, our long-term residential program provides continued therapeutic support, community, and accountability beyond the first weeks of recovery.
- Fentanyl co-occurring support: Because black tar heroin supplies are increasingly contaminated with fentanyl, our fentanyl addiction treatment team is experienced in managing polysubstance opioid dependence and the specific clinical challenges it creates.
Recovery from black tar heroin addiction is possible. Call Still Detox now at (561) 556-2677. Our admissions team is available 24 hours a day, 7 days a week to answer your questions, verify your insurance, and help you take the first step.
Frequently Asked Questions
What is the difference between black tar heroin and regular heroin?
Black tar heroin is a low-purity, minimally processed form of heroin produced mainly in Mexico and sold west of the Mississippi. Powder heroin is more refined and typically purer. Black tar carries added dangers including a uniquely high risk of wound botulism and gas gangrene linked to its production method and injection practices. Both forms carry extreme addiction and overdose risk, but black tar introduces distinct bacterial infection risks that powder heroin does not carry at the same level.
Why is black tar heroin black?
The dark color comes from the incomplete acetylation process used in production. When morphine is converted to heroin without full purification, residual byproducts, plant material, and processing chemicals remain in the final product. These impurities give it its characteristic dark brown to black color and the sticky, tar-like texture that distinguishes it from powder heroin forms.
What is black tar meth? Is it the same as black tar heroin?
No. Black tar meth and black tar heroin are completely different drugs. Black tar heroin is an impure form of diacetylmorphine, an opioid. Black tar meth refers to a dark-colored, impure form of methamphetamine, a stimulant. They belong to different drug classes with opposite effects on the central nervous system. The “black tar” descriptor in both cases refers to appearance and purity, not any shared chemistry.
Can you snort black tar heroin?
Not in its natural form. The sticky, gummy consistency of raw black tar heroin makes nasal administration impossible without drying it into a powder first. Some users do dry it and crush it for snorting, but this is far less common than injecting or smoking. All methods carry the same overdose and addiction risk. Snorting causes progressive damage to nasal tissue and the sinus lining with repeated use.
What makes black tar heroin more dangerous than powder heroin?
Beyond shared heroin risks, black tar carries a significantly elevated risk of wound botulism and gas gangrene. The drug’s crude production and transport conditions allow Clostridium botulinum spores to contaminate the supply. When injected under the skin or into muscle, these spores can germinate and release a neurotoxin that causes potentially fatal descending paralysis. Powder heroin does not carry this level of bacterial contamination risk.
What are the signs of a black tar heroin overdose?
Signs include very slow or stopped breathing, blue or gray lips and fingertips, complete unresponsiveness, gurgling or choking sounds, limp body, and pinpoint pupils even in dim lighting. Call 911 immediately and administer naloxone if available. Multiple doses may be needed if fentanyl contamination is present. Stay with the person until emergency services arrive.
How long does heroin withdrawal last?
Acute heroin withdrawal typically begins within 6 to 12 hours of the last dose and peaks at 48 to 72 hours. Most physical symptoms resolve within 5 to 7 days. Post-acute withdrawal syndrome can cause lingering depression, disrupted sleep, and recurring cravings for weeks to months afterward, particularly in long-term heavy users.
Is black tar heroin addiction treatable?
Yes. Opioid use disorder from black tar heroin is a treatable medical condition. FDA-approved medications including buprenorphine, methadone, and naltrexone are highly effective at reducing cravings, easing withdrawal, and lowering overdose risk. Combined with behavioral therapies, these treatments give people the best realistic chance of achieving and maintaining lasting recovery.
References
- Substance Abuse and Mental Health Services Administration (SAMHSA). (2021). 2020 National Survey on Drug Use and Health: Detailed tables. U.S. Department of Health and Human Services. https://www.samhsa.gov/data/release/2020-national-survey-drug-use-and-health-nsduh-releases
- Drug Enforcement Administration (DEA). (2020). Drug fact sheet: Heroin. U.S. Department of Justice. https://www.dea.gov/sites/default/files/2020-06/Heroin-2020_0.pdf
- Centers for Disease Control and Prevention (CDC). (2019). Wound botulism outbreak among persons who use black tar heroin: San Diego County, California, 2017-2018. MMWR Morbidity and Mortality Weekly Report, 67(52). https://www.cdc.gov/mmwr/volumes/67/wr/mm675152a3.htm
- National Institute on Drug Abuse (NIDA). (2021). Heroin DrugFacts. National Institutes of Health. https://nida.nih.gov/publications/drugfacts/heroin
- MedlinePlus. (2022). Substance use: Heroin. U.S. National Library of Medicine. https://medlineplus.gov/ency/patientinstructions/000798.htm
- Passaro, D. J., Werner, S. B., McGee, J., Mac Kenzie, W. R., and Vugia, D. J. (1998). Wound botulism associated with black tar heroin among injecting drug users. JAMA, 279(11), 859-863.
- American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Publishing.
- Centers for Disease Control and Prevention (CDC). (2003). Wound botulism among black tar heroin users: Washington, 2003. MMWR Morbidity and Mortality Weekly Report, 52(37), 885-886. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5237a3.htm